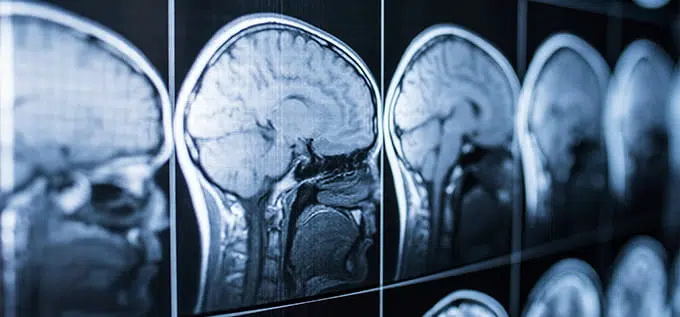
Common Brain Injury Symptoms Missed After a Car Crash
Many California car crash survivors walk away from collisions believing they escaped without serious injury. They decline the ambulance, drive home, and assume the headache or foggy feeling will pass. But traumatic brain injury symptoms often don’t appear immediately—they can develop hours or even days after the initial impact, catching people off guard when they least expect it.
Quick Answer: Subtle Brain Injury Symptoms You Shouldn’t Ignore After a Crash
After a car accident, your body floods with adrenaline and stress hormones that can temporarily mask pain and confusion. This survival response means you might feel relatively fine at the scene, only to develop concerning brain injury symptoms within the next 24 to 72 hours. Understanding what to watch for can make a significant difference in both your health outcomes and any potential legal documentation.
The most commonly missed symptoms include: new or worsening headaches that don’t respond to over-the-counter medication, dizziness or balance problems when walking or turning your head, brain fog that makes you feel slower or “not yourself,” trouble focusing on conversations or tasks at work, memory slips like forgetting recent conversations or misplacing items, irritability and mood swings that surprise you and those around you, sleep changes (sleeping far more or struggling to sleep at all), and sensitivity to light or noise that feels overwhelming.
Even low-speed collisions—including rear-end impacts at just 10 mph—can cause mild traumatic brain injury without any visible head wound, bleeding, or loss of consciousness. The sudden acceleration and deceleration forces can cause your brain to move within your skull, resulting in injury that standard CT or MRI scans may not detect immediately. Vehicle damage alone does not determine whether a brain injury occurred.
Early medical attention serves two important purposes: it allows medical providers to detect serious problems like brain swelling or blood clots, and it creates medical records that document your symptoms close in time to the crash. If symptoms worsen and you later pursue a brain injury claim, this early documentation can be valuable evidence.
If you suspect you or someone you know sustained a head injury in a California car crash, 1-800-THE-LAW2’s 24/7 accident hotline helps connect injured people with independent car accident attorneys for free consultations. These California personal injury lawyers can evaluate your situation and explain options that may be available to you.
Why Brain Injuries Are So Often Missed After a Car Accident
Traumatic brain injury TBI from car crashes is frequently overlooked in emergency rooms and by victims themselves, particularly in the critical first 24 to 72 hours after impact. This happens for several converging reasons that create a dangerous gap between the initial trauma and symptom recognition.
Adrenaline masks the damage. Immediately following a collision, your body enters fight-or-flight mode. Elevated adrenaline, endorphins, and stress hormones suppress pain perception and cloud your awareness of confusion or dizziness. You might feel shaken but alert enough to decline EMS transport or leave the scene without medical evaluation. A driver rear-ended at a stoplight on the 405, for example, might feel fine enough to exchange insurance information, drive home, and go to bed—only to wake up the next morning with a throbbing headache and difficulty remembering the details of the crash.
Standard imaging often appears normal. Concussions and other forms of mild TBI frequently don’t produce abnormalities visible on CT or MRI scans performed in emergency settings. These scans detect gross structural damage like bleeding or skull fractures but are insensitive to the microscopic brain tissue damage and neurochemical disruptions characteristic of mild traumatic brain injury. When scans return “normal,” both patients and medical professionals may conclude nothing is wrong—creating false reassurance during the window when symptoms are still developing.
Symptoms emerge gradually. Brain chemistry changes, inflammatory cascades, and swelling can take hours or days to fully develop after the initial impact. A person involved in a side-impact crash at a California intersection might experience mild dizziness at the scene, attribute it to shock, and not recognize the connection until day two or three when the dizziness worsens and balance problems make walking feel unsafe. By then, the causal link between the crash and the symptoms becomes harder to establish without early medical documentation, as outlined in many California car accident timelines.
Common Brain Injury Symptoms People Miss After a Car Crash
Brain injuries affect three major areas of function: physical sensations and abilities, thinking and cognitive processing, and mood and behavior. Injury symptoms can appear in any of these domains—or in all three simultaneously. Recognizing these patterns helps distinguish normal post-crash stress from something that warrants medical evaluation.
Physical symptoms represent your body’s direct response to brain trauma. Persistent headaches are the most frequently reported symptom, particularly throbbing or pressure-type headaches that feel different from your baseline, worsen over time, or don’t improve with typical pain medication. Dizziness and vertigo—the sensation that the room is spinning or that you’re off-balance when walking—indicate involvement of the brain’s vestibular system. Nausea or vomiting within the first 24 to 48 hours can signal neurological involvement rather than a stomach bug. Light or noise dizziness and sensitivity can make bright phone screens, sunlight, fluorescent lights, or normal background sounds feel painfully overwhelming. Unusual fatigue persists even after adequate rest, and sleep problems manifest as either sleeping much more than usual or difficulty falling and staying asleep.
Cognitive symptoms reflect injury to your brain’s processing capacity. Brain fog is often described as feeling mentally sluggish, slower than normal, or “in a cloud”—distinct from simple tiredness. Short-term memory problems appear as misplacing items repeatedly, forgetting conversations that occurred hours earlier, or asking the same questions multiple times without realizing it. Difficulty concentrating affects work performance, reading comprehension, or even following TV shows you previously enjoyed. Processing speed slows noticeably—you may struggle to respond quickly in conversations or take longer to understand directions. Word-finding difficulties make it hard to access vocabulary that should come automatically, leaving you feeling like thoughts are “stuck.”
Emotional and behavioral symptoms often surprise both the injured person and their family members. Irritability leads to snapping at loved ones over minor issues or expressing frustration disproportionate to the situation. Anxiety manifests as new nervousness or panic in situations that felt comfortable before—like riding in a car after the crash. Sadness, emotional flatness, or feeling disconnected resemble depression symptoms. Mood swings and personality changes are frequently noticed by others before the injured person recognizes them. Family may report that you “don’t seem like yourself,” are more withdrawn, or react unpredictably to normal situations.
Delayed and Subtle Symptoms: When “Feeling Off” Could Signal a Brain Injury
One of the most challenging aspects of post concussion syndrome and mild TBI is that symptoms sometimes don’t appear until days or even a few weeks after the car crash. What begins as minor discomfort can gradually escalate into problems that significantly affect daily functioning.
Symptoms often start small and build. Day one post-collision might involve a mild headache you dismiss as tension. Day two brings increasing headache and noticeable difficulty concentrating at work. By day three, you’re experiencing worsening headaches that don’t respond to medication, marked brain fog that affects job performance, and emerging balance problems. This gradual escalation means symptoms mild enough to ignore initially become undeniable within a week—but by then, connecting them to the crash requires more deliberate documentation.
Common delayed symptoms include: persistent headaches developing or intensifying several days after the accident, worsening brain fog that causes you to “space out” during conversations or while driving, struggling with work or school tasks that used to feel routine, family members noticing you seem different or more withdrawn or emotional than usual, and new difficulty tolerating screens, busy grocery stores, or loud environments that previously felt manageable.
Consider a parent in Los Angeles involved in a rear-end collision on the freeway or a driver hurt in a crash who later consults a San Bernardino car accident lawyer for help with their claim. She feels shaken but alert at the scene, declines EMS, and goes home to rest. The next day she notices mild brain fog but attributes it to just stress about the accident. Returning to work, she manages her responsibilities but with more effort—emails take longer to process, small errors appear in documents. By day four or five, she realizes she cannot maintain her previous work productivity and finally seeks medical care and consults a Los Angeles personal injury lawyer. Without early evaluation, her initial mild symptoms went undocumented, making it harder to establish a clear timeline connecting her cognitive difficulties to the crash.
Fluctuating symptom patterns add confusion. Many people experience days that feel “almost normal” followed by days that feel significantly worse. This inconsistency causes self-doubt—you may think “maybe I’m fine” on good days, then become concerned again when symptoms return with force. Family members and employers may also struggle to understand the situation when your functioning varies day to day.

Red-Flag Warning Signs: When to Seek Emergency Care Right Away
While many brain injury symptoms develop gradually and warrant urgent but non-emergency evaluation, certain symptoms after a car crash signal potentially serious complications requiring immediate medical attention. These warning signs may indicate brain swelling, bleeding, or other conditions that can become life-threatening without prompt intervention.
Seek emergency medical care or call 911 if you experience any of the following:
Loss of consciousness at any point after the crash—even briefly—warrants emergency evaluation. Sudden severe headache that worsens rapidly and doesn’t improve with rest or usual medication can indicate increasing intracranial pressure. Repeated vomiting or nausea appearing soon after the accident may signal neurological involvement. Seizures or convulsions indicate significant brain dysfunction requiring immediate intervention. Slurred speech, weakness, or numbness in the face, arms, or legs suggests potential brainstem or motor cortex involvement. Unequal pupil size or one eye appearing different from the other can indicate dangerous pressure changes. Clear fluid from the nose or ears may indicate cerebrospinal fluid leakage from a membrane breach. Extreme confusion or agitation—including inability to recognize familiar people or places—represents significant consciousness alteration.
These emergency symptoms may appear not just at the scene but hours or days afterward. Someone who seemed fine immediately following the collision might develop worsening symptoms that qualify as red flags the next morning. Delayed injuries still require urgent assessment when they progress or worsen, and understanding what to do when injured in a car accident can help you respond appropriately.
This article does not replace medical advice. Anyone experiencing these symptoms should follow recommendations from licensed healthcare providers and seek immediate medical care when warning signs appear.
Special Concerns: Children, Older Adults, and People With Prior Head Injuries
Some groups face higher risk for missed brain injuries or may display different symptoms following a car accident. Understanding these variations helps ensure appropriate care for vulnerable populations.
Children present unique recognition challenges, particularly those under age 12 who may not possess the language or self-awareness to describe headaches, dizziness, or brain fog accurately. Instead of verbal complaints, watch for behavioral manifestations: unusual fussiness or irritability, regression to earlier behaviors like thumb-sucking, changes in sleep patterns, sudden loss of interest in toys or activities, unexpected drops in school performance, or new balance problems and clumsiness. Even children properly restrained in car seats or boosters can sustain head injuries from sudden acceleration and deceleration forces. Parents and caregivers should monitor behavior closely for several days after any collision where a child’s head may have moved suddenly.
Older adults face compounding complexities because pre-existing conditions can mask or mimic new brain trauma. Seniors with baseline balance problems, mild cognitive impairment, or age-related memory changes may not recognize sudden worsening as a new injury rather than their usual symptoms. Additionally, many older adults take blood thinners prescribed for conditions like atrial fibrillation or prior stroke. These medications significantly increase the risk that even minor head trauma will produce serious bleeding complications. A relatively minor collision that causes only a small brain bleed could progress to life-threatening hemorrhage in someone on anticoagulation therapy. Any older adult involved in a motor vehicle collision should discuss the incident with their physician, even if the impact seemed minor.
People with prior concussions or brain injuries face increased vulnerability to complications from additional trauma. Research on chronic traumatic encephalopathy and cumulative brain injury indicates that each successive head injury can produce more severe effects than the previous one. The brain becomes more vulnerable after prior trauma. Anyone with documented previous concussion or TBI who is involved in a California car crash should inform their treating physician and monitor carefully for ongoing symptoms—even if normal brain function seemed restored before the new incident.
What To Do If You Suspect a Brain Injury After a California Car Crash
If you recognize any of the symptoms described above, concrete steps can help protect both your health and your potential legal options. Taking action—even days or weeks after the crash—remains valuable.
Step 1: Seek medical care promptly. It is not too late to get evaluated even if several days have passed since the collision. Depending on symptom severity, visit an emergency room (for severe symptoms like those in the red-flag section), urgent care center (for moderate symptoms like significant dizziness or persistent headache), or your primary care physician (for milder symptoms or follow-up). For broader guidance on what to do when injured in a car accident, describe the collision mechanics clearly—rear-end, side-impact, rollover—along with your head position and movement during impact, whether you lost consciousness or felt dazed, what symptoms appeared immediately versus later, and how symptoms currently affect your daily function.
Step 2: Follow all medical instructions. This includes rest recommendations (both physical and cognitive rest), prescribed medications, restrictions on work or driving, and referrals to specialists like neurologists. If your provider recommends neuropsychological testing, occupational therapy, or vestibular therapy, complete these referrals promptly. Specialist evaluations create important documentation of injury severity and impact.
Step 3: Keep a symptom journal. A simple daily record noting your symptoms, their severity, timing, and impact creates invaluable documentation. Record specific physical symptoms like headaches and dizziness, cognitive difficulties like concentration problems, emotional symptoms like irritability, missed workdays, and activities you’ve avoided or curtailed. This contemporaneous documentation—created when symptoms are fresh—proves far more credible than reconstructing timelines weeks later.
Step 4: Preserve all documentation. Gather and safely store medical records, imaging results, discharge papers, receipts for treatment, referral documentation, and specialist notes. If available, preserve photographs of vehicle damage. These materials constitute evidence of injury and treatment for any potential legal proceedings.
Step 5: Be cautious with insurance communications. Insurance adjusters may contact you to obtain statements about how you feel or what you remember. While basic cooperation is expected, consider deferring detailed statements about symptoms, medical status, or prognosis until you’ve completed initial medical evaluation and better understand your condition. As part of the broader car accident timeline from wreck to check, an independent attorney can advise on appropriate communication.
Let close family members know what to watch for—they often notice changes in mood, memory problems, or behavioral symptoms before you recognize them yourself. Their observations provide valuable corroboration of symptom severity and functional impact.
How Brain Injuries Can Affect a California Car Accident Claim
Brain injuries are substantially more complex to document than visible injuries like a broken bone or laceration. A fracture appears clearly on X-ray; brain trauma frequently produces normal-appearing imaging, invisible physical symptoms, and subjective complaints that third parties find harder to verify. This complexity means brain injury claims often face greater scrutiny.
Insurance companies commonly question several aspects: They may dispute whether delayed symptoms truly resulted from the specific collision or from other causes like stress, sleep deprivation, genetic factors, or pre-existing conditions. They may argue that early imaging was “normal,” suggesting that if scans appear clear, the injury cannot be significant. They may question whether reported work difficulties or relationship strain actually result from the brain injury rather than unrelated personal factors.
Thorough medical documentation addresses these disputes. Detailed medical records linking symptoms to the collision date and mechanics establish the causal connection. Imaging results, specialist evaluations from neurologists, and neuropsychological testing can reveal dysfunction that standard scans miss and corroborate subjective complaints with objective findings. A symptom journal documenting daily functioning changes, employer notes about performance issues, and police reports describing the crash mechanics all strengthen the documentation trail. Early diagnosis and clear medical records from visits close to the accident date carry particular weight.
Possible elements of a brain injury claim may include medical expenses such as ER visits, imaging studies, neurologist consultations, and therapy. Lost wages or reduced work hours when the injured person cannot work at full capacity deserve documentation. Future medical needs including rehabilitation, ongoing treatment, and monitoring may factor into longer-term considerations. The impact on daily life, relationships, and activities previously enjoyed represents non-economic damages that vary significantly by case, and working with the right personal injury lawyer in California can help ensure these losses are fully considered.
Each situation presents unique facts regarding collision severity, injury severity, pre-existing conditions, blood pressure and other health factors, and jurisdiction-specific legal standards. Results vary substantially, and an independent attorney in one of our network’s legal practice areas can explain how California personal injury law may apply to specific circumstances.
When to Consider Calling 1-800-THE-LAW2 About a Possible Brain Injury
You do not have to decide alone whether you have a viable claim after a suspected brain injury from a California car crash. Understanding your options is a normal and appropriate step when facing medical recovery alongside insurance questions.
1-800-THE-LAW2 is a legal referral network that helps connect injured people in California with independent personal injury attorneys for a free legal consultation. The service is available 24/7 by phone or through the online form. 1-800-THE-LAW2 itself does not provide legal services or represent clients—legal services are provided by independent attorneys in the network. Many of these attorneys work on a contingency-fee basis, meaning attorney fees are collected only if there is a monetary recovery. However, clients may still be responsible for case costs such as medical record procurement, filing fees, or expert witness expenses.
Consider reaching out if you experience: ongoing headaches, dizziness, or brain fog that symptoms persist weeks after a crash on a California road or freeway; difficulty returning to work or school due to concentration or memory problems following the collision; confusion about how to communicate with insurance companies while still undergoing treatment for suspected brain trauma; or uncertainty about whether your situation warrants legal evaluation.
Call 1-800-THE-LAW2 or complete the contact form for a free legal consultationon the website to be connected with an independent California car accident attorney who can evaluate your specific circumstances and explain options available to you. You do not have to navigate medical appointments, insurance questions, and legal concerns alone.
Disclaimer and Responsible Attorney Information
This article is for general informational purposes only and does not constitute medical advice, diagnosis, or treatment recommendation. Readers should consult licensed healthcare professionals for diagnosis and treatment of suspected brain injuries. This content also does not constitute legal advice specific to any individual’s situation. Laws vary by jurisdiction, and readers should consult an independent attorney licensed in California for legal guidance specific to their circumstances.
1-800-THE-LAW2 helps connect consumers with independent attorneys and is not a law firm. Legal services are provided by independent attorneys in the referral network. Readers can learn more about the 1-800-THE-LAW2 attorney network, its history, and how it operates. Results in legal matters vary based on the specific facts of each case, and no outcome is guaranteed.
This content was created with the assistance of AI and reviewed by humans before publication.